Fertility problems
Having fertility problems can mean you’re having trouble getting pregnant or carrying a pregnancy.
Fertility problems are also referred to as infertility or subfertility. These difficulties can affect anyone, no matter their sex or age.
If you’ve tried to get pregnant for a year or more by having regular, unprotected sex, and you’ve not been successful, you can contact your GP for advice.
If you or your partner are over 35, or if you think that one of you might have a problem that's affecting fertility, you can see your GP after 6 months of trying.
What causes fertility problems?
Around 1 in 7 couples in the UK may have fertility problems. Many go on to conceive, with or without treatment.
It can be difficult to understand what is causing fertility difficulties. For 25% of couples who are having trouble, no clear reason is found.
Problems with ovulation
Low or reduced fertility, known as subfertility, is most often caused by problems with ovulation - the stage when the body releases an egg. Usually, this happens once a month. But if there are issues, it might mean that eggs are being released less often, or not at all.
This can be because of:
polycystic ovary syndrome (PCOS) where small growths or cysts can stop or slow the release of the egg
endometriosis, where small pieces of womb lining start growing in other places such as on the ovaries
thyroid problems, which can prevent ovulation
If you’ve just stopped using contraception, it can take time for some types, like the injection, to stop working and for your menstrual cycle to return to normal.
Problems with sperm count
Another common cause of fertility problems is poor-quality semen or a low sperm count. This means there’s not as much sperm as usual when you ejaculate (come). Up to 1 in 5 young men find they have a low sperm count. For up to 20% of couples who struggle to conceive, low sperm count is the cause of the problems.
Low sperm count could be caused by various factors, including:
a hormone imbalance such as hypogonadism, where the testicles produce few or no hormones
an inherited genetic problem
undescended testicles
a problem with the male genital tract – for example, the tubes that carry sperm can be damaged and blocked by illness or injury
a genital infection or condition such as chlamydia, gonorrhoea, prostatitis or varicocele (dilated veins within the testicles)
As a couple
You could also experience fertility problems if one of you has had:
surgery that may have scarred or affected your reproductive organs
some medications and treatments, including testosterone replacement, steroids or chemotherapy
complications in previous pregnancies or births
a sexually transmitted infection (STI), such as chlamydia or gonorrhoea
pelvic inflammatory disease (PID)
Your lifestyle can also affect your fertility. Smoking, drinking alcohol, being overweight and stress can all affect your chances of conceiving. Smoking can reduce sperm count, though it should increase again after quitting.
Age and fertility
Fertility in women and people with ovaries starts to decrease in the mid-thirties. For men and people with penises, the decrease starts at age 40–45.
These figures show the typical chance of conceiving at different ages.
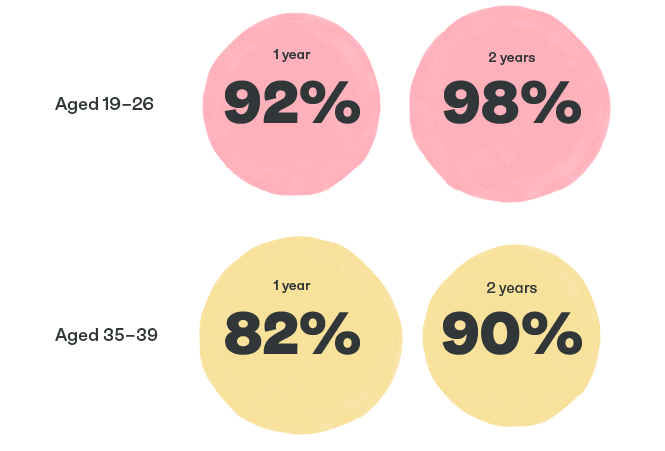
Age 19-26: Typically 92% of people in this group get pregnant after 1 year of trying. And 98% of them get pregnant after trying for 2 years.
Age 35-39: Typically 82% of people this age will get pregnant in 1 year of trying. And 90% will get pregnant when trying for 2 years.
Getting tested
When you first seek advice from a fertility clinic or GP, the clinician may recommend you keep trying for a while if you’ve been having regular, unprotected sex for less than a year.
If you've been trying for more than a year, your clinician may recommend a range of tests to find out what's stopping you from conceiving. You may also be offered counselling.
A number of tests can be used to try and understand the cause of fertility problems:
physical examination - a clinician will check the penis and testicles for anything unusual, including lumps and signs of infection
hormone tests – a clinician will take a blood sample to check the hormones that affect ovulation
checking your ovaries – this could be a blood test or an ultrasound scan to examine your ovaries for any problems
semen analysis – this looks at a small sample of semen (ejaculate) and checks the sperm count and if the sperm are moving around correctly. You might be asked to stop having sex for a few days before the test to ensure you can produce enough semen.
STI test – untreated chlamydia and gonorrhoea can cause problems with conceiving. If you have an infection, you’ll be prescribed antibiotics to treat it
hysterosalpingogram (HSG) – this is an x-ray of the womb and fallopian tubes. A special dye is inserted before the x-ray is taken, to help show up any problems like a blockage of the fallopian tubes
hysterosalpingo-contrast-ultrasonography (HyCoSy) – an ultrasound scan that uses a small amount of fluid to check if fallopian tubes are damaged or blocked
laparoscopy – a clinician will make a small cut in your lower abdomen (tummy), then use a thin, tubular telescope to look at your womb, fallopian tubes and ovaries. This is usually carried out under general anaesthetic and is only used if there is a high chance that there is an internal problem
Considering treatments
Whether or not a clear cause is found, your clinician or GP can talk you through the next steps. This may include a referral for further investigation or treatment.
The fertility treatment available through the NHS will depend on where you live in the UK. The treatment available, and who is eligible for it, varies. And waiting lists for treatment can be long in some areas.
You may wish to pay for treatment privately. Make sure you research clinics carefully. Any price quotes should include all costs and details of treatment options. Choose a private clinic that is licensed by the Human Fertilisation and Embryology Authority (HFEA), which regulates and inspects fertility clinics in the UK.
Treatments could include medicine to improve fertility, for example, to stimulate ovulation. Depending on any issues that may have been found, surgery may be an option, for example, to repair damage to the fallopian tubes. Or you may be advised about different options for assisted conception.
Do you need help with something else?
Find sexual health services near you
Get sexual health advice from the experts




